Daniel Mirea (March 2026)
NeuroAffective-CBT® | https://neuroaffectivecbt.com
Abstract
NeuroAffective Narrative Reconsolidation (NNR) is a trauma-processing method developed within the NeuroAffective-CBT® (NA-CBT®) framework. The approach integrates principles from trauma-focused cognitive behavioural therapy, affective neuroscience, and dual-attention trauma processing to enable clients to revisit traumatic memories while maintaining physiological regulation and present-moment awareness.
Unlike interventions that focus primarily on cognitive restructuring, NNR emphasises the coordinated engagement of physiological regulation, affective processing, and narrative meaning-making. The model assumes that traumatic memories often persist because they remain encoded as ongoing threat experiences rather than integrated autobiographical events.
The central therapeutic objective of NNR is the development of what NA-CBT conceptualises as the Integrated-Self, a state in which traumatic experiences can be recalled without triggering overwhelming emotional or physiological responses. Through structured cycles of narrative activation, somatic tracking, distress modulation, and identity integration, the intervention aims to facilitate memory reconsolidation and transform trauma memories into coherent elements of personal narrative.
This article outlines the theoretical foundations of NNR and situates the method within the broader NA-CBT treatment framework. A detailed clinical case illustration then demonstrates how trauma memories may gradually shift from overwhelming threat experiences toward integrated life events, supporting the emergence of a more stable and resilient sense of self. The clinical implications of this approach and its relevance for future research on trauma integration and memory reconsolidation are also discussed.
Keywords
NeuroAffective-CBT; trauma therapy; memory reconsolidation; affect regulation; narrative integration; interoception; PTSD; autobiographical memory; Integrated-Self; psychotherapy integration.
Introduction: Trauma Beyond Cognition
Cognitive-Behavioural Therapy (CBT) remains one of the most empirically supported psychological treatments across a wide range of mental health disorders. Its strength lies in its structured, transparent, and collaborative focus on the relationships between thoughts, behaviours, and emotional responses. Yet over the past two decades, developments in neuroscience and trauma psychology have increasingly highlighted something clinicians have long observed in practice: emotional suffering cannot be fully explained, or resolved, through cognition alone.
Trauma illustrates this limitation particularly clearly. Clients frequently report that they intellectually understand that the event is over, yet their bodies continue to react as if the threat were still present. Their heart rate accelerates, their stomach tightens, breathing becomes shallow, and muscles brace defensively, sometimes before a conscious thought has formed. Insight may be present, yet the nervous system remains unconvinced.
NeuroAffective-CBT was developed in response to this clinical reality. The model represents an integrative therapeutic framework that combines insights from affective neuroscience, physiological regulation, and cognitive-behavioural therapy into a unified approach to emotional distress. Within NA-CBT, psychological suffering is conceptualised as emerging from dysregulation within a body–brain–affect system, in which physiological arousal, emotional experience, and cognitive interpretation continuously interact.
From this perspective, the brain functions fundamentally as a predictive organ. Its primary task is not abstract reasoning but survival. It constantly evaluates whether the organism is safe. When physiological signals, such as increased heart rate, muscle tension, pain, or breathlessness, indicate possible danger, the brain rapidly amplifies threat interpretations. These interpretations reinforce anxiety, avoidance, hypervigilance, and negative beliefs about the self or the world. Over time, this cycle may become self-perpetuating.
Therapeutic change therefore cannot rely solely on cognitive restructuring. If the body continues to generate threat signals, cognition is placed in a reactive position, attempting to reason with an alarm that has already been activated. Sustainable recovery requires coordinated regulation of physiology, affect, and cognition. It involves helping the nervous system experience safety while traumatic memories are revisited.
Integration Within NA-CBT
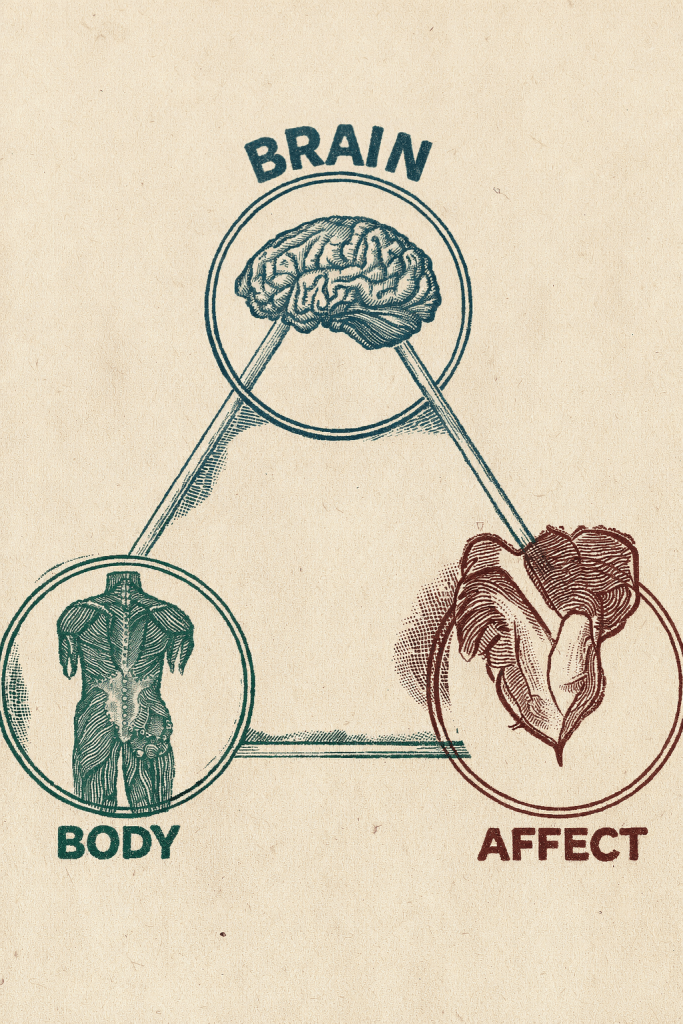
NeuroAffective-CBT synthesises several theoretical influences into a coherent clinical framework. Rather than treating cognition, emotion, and physiology as separate domains, the model conceptualises them as interacting components of a single regulatory system. This perspective is captured in what NA-CBT describes as the Body–Brain–Affect model (Figure 1), a central conceptual element that illustrates how emotional experience emerges through the continuous interaction between physiological signals, emotional states, and cognitive interpretation.
Within this framework, physiological signals from the body influence emotional states, which in turn shape cognitive interpretations of threat and safety. When the body signals danger through pain, tension, or heightened arousal, the brain rapidly generates emotional responses that influence perception and thought. Conversely, cognitive interpretations may amplify or soothe emotional responses, which subsequently feed back into physiological regulation.
From a therapeutic perspective, this triangle highlights an essential principle: effective treatment must address all three domains simultaneously. Improvements in physiological regulation often reduce emotional reactivity, making cognitive updating more accessible. Changes in cognitive interpretation may soften emotional responses and allow the body to relax. Likewise, emotional processing occurring within a safe relational context may enable both physiological and cognitive systems to reorganise.
Within NA-CBT, this integrated understanding forms the conceptual foundation upon which later treatment modules, including trauma processing through the NeuroAffective Narrative Reconsolidation (NNR) protocol, are built.
Treatment Structure of NeuroAffective-CBT
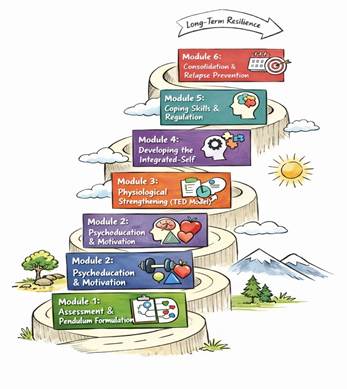
NA-CBT is delivered through six sequential treatment modules designed to progressively stabilise physiological regulation, before processing traumatic experiences, in order to consolidate long-term psychological resilience. Each module builds upon the previous phase, moving from assessment and stabilisation toward trauma integration and relapse prevention (Figure 2).
Module 1: Assessment and the Pendulum-Effect Formulation
Comprehensive clinical assessment focusing on predisposing, precipitating, perpetuating, and protective factors. Development of the NA-CBT pendulum formulation mapping oscillations between three main self-sabotaging strategies: avoidance, overcompensation, and capitulation (in no particular order).
Module 2: Psychoeducation and Motivation
Introduction to the Body–Brain–Affect model and the pendulum-effect framework. Psychoeducation about physiological regulation, trauma responses, and the interaction between cognition, affect, and bodily states.
Module 3: Physiological Strengthening (TED Model)
Stabilisation of biological rhythms through the TED (Tired-exercise-Diet) model and in the case of traumatic exposure TED 2.0 (Train–Eat–Dream), emphasising sleep regulation, physical activity, and nutritional stability as foundations for emotional regulation. TED can be expanded to work with various conditions.
Module 4: Developing the Integrated-Self
Trauma processing through the NeuroAffective Narrative Reconsolidation (NNR) protocol, integrating narrative activation, somatic tracking, distress modulation, and identity reconstruction.
Module 5: Coping Skills
Development and generalisation of adaptive coping strategies and cognitive-behavioural skills to support resilience in everyday situations.
Module 6: Consolidation and Relapse Prevention
Integration of therapeutic gains, future-oriented planning, and relapse prevention strategies to maintain long-term emotional stability.
NeuroAffective-CBT: Theoretical Foundations
The theoretical foundations of NeuroAffective-CBT draw upon several complementary areas of psychological and neuroscientific research. Rather than positioning itself as a replacement for cognitive-behavioural therapy, NA-CBT extends the traditional model by integrating insights from attachment theory, affective neuroscience, trauma memory research, and identity psychology.
These perspectives converge around a central clinical observation: emotional suffering rarely arises from cognition alone. Instead, it emerges through the interaction between biological regulation, emotional processing, and personal meaning.
Trauma may be understood, at its most fundamental level, as an adaptive alert system. When an individual experiences or witnesses a life-threatening situation, the brain, whose primary function is survival, encodes the event in ways that allow future detection of similar danger. From that point onward, the nervous system becomes sensitised to cues associated with the original threat, generating anticipatory anxiety and protective vigilance aimed at preventing further harm.
Under most circumstances, this mechanism serves an adaptive purpose. However, post-traumatic stress symptoms may develop when autobiographical memory becomes disorganised and the individual’s interpretation of the event shifts toward a pervasive sense of vulnerability or incapacity (e.g., I cannot cope with similar threats). In such cases, the trauma narrative may contribute to a destabilised sense of identity, often expressed as a feeling that “I am no longer the person I used to be”.
Importantly, not every individual exposed to a frightening event develops trauma-related symptoms. Vulnerability to post-traumatic stress is influenced by multiple factors, including early developmental experiences, pre-existing cognitive schemas, attachment patterns, and available social support. Nevertheless, the capacity to generate fear responses to predicted danger is deeply embedded within mammalian neurobiology. The difference between adaptive fear and persistent trauma lies in how the experience becomes encoded, interpreted, and integrated within the individual’s broader autobiographical narrative.
Within this broader framework, specific therapeutic procedures are required to translate these principles into clinical practice. It is within this theoretical context that the NeuroAffective Narrative Reconsolidation (NNR) protocol emerges as a clinical method for trauma processing.
Attachment, Development, and Coping Patterns
From the perspective of NA-CBT, the brain’s primary survival functions begin long before conscious reasoning develops. Early relational experiences shape how the nervous system learns to detect safety and danger. Attachment theory has long helped psychotherapists understand patterns of emotional regulation, dependency, avoidance, and relational security.
Within NA-CBT, attachment styles are understood as patterns emerging from the interaction between the child’s developing neurobiology and the caregiving environment. Early experiences of emotional attunement, neglect, predictability, or threat become encoded not only as autobiographical memories but also as physiological patterns of emotional regulation.
Children raised in predictable and responsive environments typically develop nervous systems that expect safety and connection. Conversely, environments characterised by emotional neglect, inconsistent care, or exposure to threat may shape nervous systems that become chronically vigilant, avoidant, or defensive.
For this reason, developmental history plays a meaningful role in the assessment phase of NA-CBT. Childhood narratives are explored not for their own sake, but because they often illuminate how individuals learned to regulate emotion, seek support, or defend themselves psychologically.
In clinical practice, assessment therefore becomes a collaborative process of guided discovery rather than a mechanical checklist. Therapists listen for several interacting domains that help organise the client’s story: predisposing factors, precipitating events, perpetuating mechanisms, and protective factors. Understanding these domains allows clinicians to appreciate not only what has contributed to distress but also what strengths remain available within the client’s life narrative.
Affective Neuroscience
Insights from affective neuroscience further clarify why cognitive insight alone is often insufficient to resolve trauma-related distress. Emotional responses frequently originate in subcortical threat-detection systems that operate rapidly and automatically, often before conscious cognitive appraisal occurs (LeDoux, 2015). These neural systems evolved to prioritise survival and are therefore highly sensitive to signals of danger.
As a result, trauma memories are rarely encoded as purely verbal or conceptual experiences. Instead, they are often stored as multisensory experiences involving bodily sensations, emotional states, and perceptual fragments. A racing heart, tightening stomach, or sudden surge of fear may therefore occur even when the individual rationally understands that the present moment is safe.
Recognising this helps explain why therapeutic approaches that incorporate physiological awareness and regulation often prove more effective in trauma work than those relying solely on cognitive dialogue.
Trauma Memory Models
The cognitive model of post-traumatic stress disorder proposed by Ehlers and Clark (2000) provides another important theoretical foundation for NA-CBT. According to this model, trauma symptoms persist when memories of the event remain insufficiently integrated within autobiographical memory.
Rather than being recognised as events that occurred in the past, trauma memories are experienced as ongoing threats in the present.
In practice, this means that reminders of the trauma, sounds, bodily sensations, environments, or thoughts, can reactivate the original threat response. Individuals may experience intrusive recollections, flashbacks, or intense emotional reactions that feel immediate and overwhelming.
From a NeuroAffective perspective, these responses reflect the nervous system’s difficulty distinguishing between memory and present danger.
Shame and Self-Identity
Traumatic experiences frequently influence identity as much as emotional regulation. Research on shame and vulnerability demonstrates how adverse experiences can reshape the narratives individuals hold about themselves (Brown, 2012). Traumatic events are not only remembered as external occurrences but are often internalised as reflections of personal inadequacy or vulnerability.
A traumatic event may give rise to beliefs such as I am weak, I am permanently damaged, I am ashamed of what happened, or I cannot trust the world. These identity-based interpretations may become deeply embedded, shaping behaviour, expectations, and interpersonal relationships long after the original event has passed.
Within the NA-CBT framework, attention to identity narratives therefore becomes an essential component of trauma recovery. Therapeutic work involves not only reducing fear responses but also helping clients reconstruct a coherent and compassionate understanding of themselves.
Addressing internalised shame is particularly important in this process. Shame can be understood as a socially mediated form of threat response, involving fears of rejection, exclusion, or negative evaluation by others. It is frequently associated with beliefs about being fundamentally flawed, socially rejected, or unworthy of acceptance. When such beliefs remain unexamined, they may perpetuate avoidance, withdrawal, and emotional dysregulation. Bringing these shame-based narratives into conscious awareness within the safety of a supportive therapeutic context, allows them to be re-evaluated and integrated, thereby supporting both emotional regulation and identity reconstruction.
Memory Reconsolidation
Neuroscience research on memory reconsolidation provides an additional explanatory framework for therapeutic change. Traumatic experiences are often encoded under conditions of intense emotional arousal, which can disrupt the normal integration of sensory, emotional, and contextual information. As a result, trauma memories may be stored in fragmented or poorly integrated forms, contributing to disorganised recollection and intrusive re-experiencing.
Research suggests that when emotional memories are reactivated under conditions of relative safety, they temporarily enter a labile state in which they can be modified before being stored again, a process referred to as memory reconsolidation (Lane et al., 2015; Nader and Hardt, 2009). During this window, new emotional or contextual information may become incorporated into the existing memory trace.
Within therapy, revisiting traumatic memories in a regulated and supportive context may therefore allow the nervous system to encode new emotional associations alongside the original experience. The event remains remembered, but its emotional intensity and subjective meaning may gradually change.
Dual-Attention Processing
Traumatic experiences are frequently encoded under conditions of extreme threat, during which heightened physiological arousal and stress hormones can narrow attentional focus toward the perceived source of danger. As a result, individuals often recall highly salient threat-related details while other contextual information remains poorly encoded. For example, victims of violent assault may vividly remember the weapon involved while recalling relatively few details about the surrounding environment.
Trauma therapies such as Eye Movement Desensitisation and Reprocessing (EMDR) emphasise the importance of maintaining simultaneous awareness of the traumatic memory and present-moment safety. This process, often described as dual-attention, allows individuals to revisit distressing memories while remaining oriented to the current environment and the therapeutic relationship (Shapiro, 2018).
Maintaining this broader attentional field may help prevent full re-immersion in the traumatic experience. Instead, the memory is held within a wider context that includes bodily regulation, environmental orientation, and cognitive reflection. This expanded awareness may support the integration of previously inaccessible contextual information, allowing fragmented memories to be reorganised into a more coherent autobiographical narrative.
Core Principles of NeuroAffective Narrative Reconsolidation (NNR)
NeuroAffective Narrative Reconsolidation (NNR) is guided by several core therapeutic principles derived from cognitive-behavioural trauma models, affective neuroscience, and memory reconsolidation research. First, traumatic memories must be sufficiently activated for the underlying memory network to become accessible for modification. Second, this activation must occur under conditions of physiological regulation and interpersonal safety, allowing the nervous system to remain within a tolerable window of emotional engagement. Third, therapeutic change occurs when new contextual, emotional, and cognitive information becomes integrated into the reactivated memory trace.
Within NA-CBT, this process is supported through the coordinated engagement of narrative activation, somatic awareness, distress modulation, and identity reconstruction. Rather than focusing exclusively on cognitive reinterpretation, the NNR protocol emphasises the simultaneous regulation of physiological arousal, emotional processing, and autobiographical meaning. Through repeated cycles of regulated memory activation and updating, traumatic experiences can gradually shift from present-tense threat states toward integrated autobiographical memories.
NeuroAffective Narrative Reconsolidation and the Integrated-Self
It is within this theoretical context that the NeuroAffective Narrative Reconsolidation (NNR) protocol was developed. NNR represents the primary trauma-processing intervention used in Module 4 (out of 6) of NA-CBT, the module referred to as Developing the Integrated-Self.
The aim of NNR extends beyond simple symptom reduction. Its deeper objective is integration. Within NA-CBT, the Integrated-Self refers to a psychological state in which traumatic experiences are incorporated into autobiographical narrative rather than experienced as ongoing threats. The memory remains accessible, but it no longer carries the same physiological urgency or identity-disrupting meaning. The individual can look back without being pulled back into the emotional state of the original event.
NNR draws upon several established therapeutic mechanisms. From trauma-focused CBT it incorporates imaginal reliving, hotspot identification, and cognitive updating. From EMDR-informed approaches it adopts the principle of targeted memory activation combined with dual attention, maintaining awareness of both the traumatic memory and present-moment safety. From affective neuroscience it integrates interoceptive awareness and autonomic regulation.
What distinguishes NNR is the deliberate sequencing and simultaneous engagement of these processes within a coherent and relationally grounded therapeutic framework.
This article presents NNR through a clinical case illustration. Rather than outlining the protocol in purely procedural terms, the case demonstrates how the method unfolds in practice: how physiological stabilisation prepares the ground for memory activation, how distress modulation creates the conditions for reconsolidation, and how identity integration transforms the meaning of trauma without denying its reality.
The case illustration presented later in the article demonstrates how the Integrated-Self may emerge through a carefully guided reconnection between body, affect, and autobiographical narrative.
Why the Integrated-Self Matters
Following trauma, many individuals report not only fear-related symptoms but also a disruption in their sense of identity continuity. They often describe an internal division between the person I was before and the person I am now. Even when external functioning appears intact, the trauma may persist internally as an unintegrated chapter that intrudes into the present through physiological surges, intrusive imagery, avoidance patterns, and shifts in self-appraisal.
From an NA-CBT perspective, this represents not merely a problem of memory content but of memory status. A trauma memory that remains “threat-coded” functions like an alarm in the present rather than a narrative of the past. The individual may be able to describe the event factually, yet the nervous system responds as though the danger is occurring again. This disrupts meaning-making, reduces agency, and often reshapes identity through interpretations such as I am unsafe, I am weak, or I cannot trust my body.
Within NA-CBT, the Integrated-Self refers to the stage at which traumatic experiences can be recalled without triggering a present-tense threat response. The event is neither erased nor minimised. Instead, it becomes located appropriately in time and meaning, an autobiographical memory rather than a re-lived danger state. The individual can look back without being pulled back into the emotional state of the original event.
Accordingly, the therapeutic aim is not to eliminate memory but to achieve integration: restoring continuity of self, updating meaning, and enabling the nervous system to learn, through experience rather than instruction, that the present is no longer the past.
A NNR Protocol for Trauma Processing
When clinicians and clients speak about “processing trauma”, it is often imagined as a primarily cognitive task: challenging beliefs, reframing interpretations, or practising coping statements. In clinical reality, however, trauma is rarely represented only in language. It is frequently expressed first through physiology, tightness in the chest, visceral constriction, trembling, heat surges, bracing muscles, and rapid shifts in breathing, often occurring before explicit meaning is consciously formed. Cognition then attempts to make sense of a state the nervous system has already entered: “I am not safe”.
NeuroAffective-CBT was developed with this premise at its core. The model assumes that post-traumatic distress is not a single-system phenomenon but an ongoing interaction between social context, physiology, affect, and cognition, each shaping the others in real time. Humans are fundamentally social organisms, and the relational environment in which trauma is revisited therefore plays a crucial therapeutic role. Particular attention is given to the authenticity and safety of the relationship between therapist and client. Clinical experience and psychotherapy research suggest that outcomes are strengthened when clients experience the therapist as both professionally competent and interpersonally safe, particularly in trauma work where shame and threat sensitivity may be elevated. Within a safe therapeutic relationship, clients are often better able to confront painful memories while reducing the shame and self-judgement that frequently accompany traumatic experiences.
If trauma is encoded and maintained across social, physiological, affective, and cognitive systems, recovery must engage these systems together, coordinating bodily regulation, affect tolerance, and narrative meaning-making within a single therapeutic process.
Within Module 4 of NA-CBT (Developing the Integrated-Self), this coordinated process is operationalised through NeuroAffective Narrative Reconsolidation. NNR is not a simple combination of CBT and EMDR techniques, nor a rebranding of existing trauma protocols. Rather, it is a structured method for integrating traumatic memories into autobiographical narrative while maintaining sufficient regulation to allow updating and reconsolidation to occur without overwhelming the client.
The sections below clarify why the concept of the Integrated-Self is clinically relevant and outline the mechanistic logic that informs the NNR protocol.
The Rationale of NeuroAffective Narrative Reconsolidation
NNR is guided by a principle shared across cognitive and neurobiological trauma models: when a memory is reactivated under conditions of safety, it becomes available for updating. Trauma processing therefore requires more than recall; it requires recall paired with regulation and new information.
In cognitive-behavioural terms, this includes imaginal reliving, hotspot identification, cognitive updating, and meaning reconstruction. In EMDR-informed terms, it echoes the principle of dual attention: the capacity to keep one “foot” in the memory while maintaining connection to the present environment and the therapeutic relationship. In NA-CBT terms, it is a body–affect–meaning integration process: the therapist tracks how the body responds, supports affect tolerance, and facilitates narrative updating in ways that are congruent with physiological state.
The distinctive contribution of NNR is not any single element. It is the deliberate sequencing and simultaneous engagement of core mechanisms, narrative activation, somatic tracking, distress modulation, perspective shifting, identity reframing, and future orientation, within a coherent arc designed to support reconsolidation rather than retraumatisation.
NNR assumes that effective trauma processing requires three conditions:
- Sufficient activation of the target memory (so the network is accessible for modification).
- Sufficient regulation (so activation remains within a tolerable window and does not collapse into overwhelm or dissociation).
- Sufficient updating information (so the memory can be re-encoded with new context, meaning, and embodied safety).
Within NA-CBT, Modules 1–3 (see treatment pathway above) function as preparation for this work by strengthening regulation capacity and stabilising the threat–safety pendulum. NNR is then introduced when the client can reliably engage regulation strategies and remain oriented to the present while recalling distressing material.
Overview of the NNR Clinical Sequence
Although adapted to individual presentation, NNR typically follows a replicable structure:
- Narrative activation of the event in present-tense or vivid recall.
- Somatic tracking of physiological shifts and localisation of distress.
- Hot memory selection to target the most emotionally loaded moment.
- Distress modulation using breathing, grounding, and imagery (e.g., dial/clock reduction) to bring arousal into a tolerable range.
- Perspective shifting (observer stance; widening context; noticing safety cues).
- Cognitive updating by incorporating new interpretations, information, or corrective emotional experience.
- Identity reframing linking the event to resilience-based self-meaning (without denial of harm).
- Values and meaning integration, where relevant, to stabilise new schemas.
- Future orientation and relapse planning to consolidate learning and reduce avoidance.
This structure ensures that memory activation is not merely endured but actively transformed, experienced within a context of regulation, updated meaning, and a revised identity narrative consistent with psychological integration.
Rationale for the Case Illustration
The remainder of this article illustrates the NNR protocol through a clinical case example. Rather than presenting the method solely in procedural terms, the case demonstrates how the intervention unfolds moment-to-moment in practice. In particular, it illustrates how physiological stabilisation prepares the ground for memory activation, how distress modulation supports tolerable engagement with traumatic material, and how identity integration can transform the meaning of trauma without denying the reality of the event.
The case that follows illustrates how the Integrated-Self can emerge through a carefully guided reconnection between body, affect, and autobiographical narrative.
A case illustration: “Edward”
“Edward” (pseudonym) was a physically active 19-year-old man who presented with persistent trauma symptoms following a severe abdominal injury sustained during a boxing sparring session. The injury led to emergency hospital treatment and surgical removal of his spleen. In the months that followed he experienced intrusive recollections, anxiety around medical environments, avoidance of contact sport, reduced confidence, and a sense that his future had narrowed. His identity, previously anchored in physical competence and sport, felt disrupted, as though his body had become unfamiliar territory.
During the initial sessions of NA-CBT, the therapeutic focus was on preparation. This included developing a collaborative relationship, a shared formulation (the pendulum-effect), mapping maintenance patterns, strengthening physiological and emotional regulation capacities. Such preparatory work is essential; without it, trauma processing can lead to excessive activation without sufficient containment, potentially leaving the client more overwhelmed than before therapy began.
By the time we entered Module 4, Edward had established a trusting bond with the therapist and could already recognise how his vulnerability, the sense of being weaker, more exposed, less “himself”, was perpetuated by what NA-CBT calls the Pendulum-effect (formulation). He oscillated between three coping modes. There was overcompensation: keeping constantly busy so his mind didn’t return to the event, working hard and filling time to outrun memory. There was hypervigilant avoidance: scanning for danger, steering away from reminders, refusing situations where he might feel physically threatened, even avoiding looking at or touching the scar. And there was capitulation: collapsing into self-criticism and shame when he noticed he had withdrawn again, telling himself he was “weak” for struggling.
From a therapeutic perspective, the autobiographical split was immediately apparent: what I am now is not who I was. And while the self-sabotaging patterns were predictable, they did not feel chosen. They felt automatic, rather than a set of strategies he was consciously selecting.
This is precisely where Integrated-Self work begins: stabilising the pendulum enough that the client can look back without being pulled under.
Disclaimer: Details of individual cases have been modified to protect confidentiality while preserving the clinical process described.
The NNR session: opening the memory, keeping the body safe
When trauma processing began, Edward was invited to recount the event as if it were occurring in the present moment.
The use of present-tense narrative was intentional. Trauma memories are not typically stored as structured verbal narratives but rather as multisensory experiences involving bodily sensations, emotions, and perceptual fragments. Present-tense recall helps reactivate the memory network in a way that resembles its original encoding, thereby making it accessible for therapeutic updating.
As Edward narrated the event, attention was repeatedly redirected toward bodily sensations. He was asked to notice where distress appeared in his body, what sensations changed, and how his physiological state shifted as the memory unfolded. Where does he feel it? What changes? What tightens? What heats? What collapses? The distress was primarily located in the central body, where the surgery scar was also located, manifesting as strong tension at the front of the upper torso, concentrated around the scar area. Edward was asked to rate the distress on a 0–10 scale, in order to track the intensity of the physiological response and to also establish a shared language for tracking regulation and change, observing shifts in emotional activation throughout the session, rather than becoming lost inside them.
Two highly distressing “hot memories” emerged quickly. One was the moment he was punched in the abdomen. The other was later, in hospital, when he was told that his spleen would need to be surgically removed. Both were highly activating: the hospital memory reached 10/10, while the punching memory was rated slightly lower at 9.5/10.
At this point an important clinical step occurred. Edward was invited to choose which memory he wished to process first, the one that felt most pressing or manageable to approach in the current session. He selected the hospital moment.
This choice was clinically significant. Trauma frequently involves experiences of helplessness or loss of control; inviting the client to select the focus of processing helps restore a sense of agency precisely where trauma had removed it.
Dialling Down Distress: Clock Imagery and Physiological Regulation
Before further processing, the focus shifted toward physiological regulation. Grounding breathwork, progressive muscle relaxation, and body-scanning exercises were introduced, followed by an imagery technique commonly used within NA-CBT trauma work: clock-dial imagery (see Figure 3).
Distress modulation is normally facilitated through a guided imagery technique referred to in NA-CBT as NeuroAffective Distress Modulation, also described as the clock-dial regulation method. The technique invites clients to imagine gradually reducing physiological arousal by “turning down” an internal dial while synchronising the imagery with slow exhalation and bodily relaxation.
The idea is simple yet clinically effective. With each slow exhalation, the client imagines turning a dial downward, from 10 to 9, from 9 to 8, and progressively lower, until the level of distress reaches 5 or below. In early sessions, it may be unrealistic to expect distress to fall substantially below SUD 5, particularly when the target memory is highly activating. The reduction in distress is guided by the natural rhythm of breathing and gradual physiological settling.

Figure 3 describes the NeuroAffective Distress Modulation or Clock-Dial Technique: a guided imagery method in which clients synchronise slow exhalation with an imagined reduction in distress (e.g., from SUD 10 toward SUD 5). Gentle hand movements may be used to embody the “dialling down” action while maintaining relaxed posture and minimal muscular effort.
During this process, Edward was encouraged to imagine physically turning the dial with his hands and/or outbreath. In some cases, the imagery may be paired with gentle physical movement: clients raise their hands slightly during inhalation and, during exhalation, allow the hands to lower naturally as if turning the dial downward, gradually reducing the intensity of distress with each out-breath. If physical movement is introduced, it is important that it remains relaxed and free of muscular strain, and that it does not distract from the primary purpose of the exercise, facilitating physiological regulation and emotional settling.
This imagery serves a specific therapeutic function. It provides traumatised individuals with a felt sense of influence over emotional intensity. Clients sometimes describe this experience as gaining “control,” but the therapeutic aim is more accurately described as restoring agency rather than suppressing emotional responses. In this sense, the imagery functions as a bridge between cognitive intention and bodily regulation, an internal interface through which the client can actively modulate physiological arousal.
As Edward practised the technique, his distress gradually reduced to approximately SUD 5 (SUDS; 0-10). The decision to pause at this level was deliberate. The aim was not to eliminate emotional activation but to maintain it within a tolerable window of engagement, where emotional processing and cognitive updating could occur without overwhelming the client.
Importantly, subjective distress ratings do not always correspond precisely with observable physiological responses. For this reason, the therapist also monitored behavioural and physiological cues such as breathing patterns, muscular tension, and posture. At one point, for example, the therapist noted persistent tension in Edward’s shoulders and continued constriction in his breathing. Edward was therefore gently invited to re-evaluate his distress rating: “I notice your shoulders are still quite tense and your breathing appears somewhat restricted. Are you sure the level has come down to five? If not, that is completely normal… we can take another moment and continue the exercise”.
Such moments of collaborative checking help ensure that regulation reflects genuine physiological settling rather than a cognitive attempt to “perform well” in therapy.
At this stage, the NNR protocol shares certain conceptual similarities with trauma-processing principles used in EMDR. Rather than maintaining narrow attentional focus on the traumatic image, the intervention deliberately expands awareness. Edward remained connected to the memory while simultaneously anchoring his attention in his breathing, bodily sensations, and the present therapeutic environment.
This broader attentional field allowed the nervous system to begin learning a crucial distinction: the memory was being recalled, but the threat itself was no longer present.
The imagery used during this phase of processing serves two primary functions. First, it should help reduce physiological arousal by activating calming imagery that signals safety to the body–brain–affect system. Second, it should be meaningful to the individual client. Imagery is therefore tailored to the client’s personal preferences, cultural background, and sources of relaxation or comfort.
Research on mental imagery in psychotherapy suggests that individuals can generate vivid internal scenes that promote emotional regulation and self-soothing (Hackmann, Bennett-Levy and Holmes, 2011). These images often engage multiple sensory modalities and may involve colours, sounds, smells, bodily sensations, or environmental scenes associated with safety and calm. Activating such multisensory representations may facilitate parasympathetic regulation and the release of endogenous opioids such as endorphins, contributing to subjective feelings of relaxation.
Assessing protective factors early in therapy can therefore provide therapists with valuable cues for identifying imagery that may support regulation and resilience during trauma processing.
Shifting Perspective: Widening the Narrative Context
Once distress had reduced to a manageable level, Edward was invited to revisit the hospital scene from an observer perspective. To support this process, we briefly located the hospital using Google Street View. The purpose was not to intensify exposure, but to help the brain anchor the memory within a concrete, real-world context, a place that exists in the external world, rather than an internal space repeatedly reactivated by flashbacks.
This step is not intended as a distraction, nor as an attempt to impose forced positivity. Rather, it functions to widen attentional focus, allowing the brain to encode contextual information that may not have been accessible during the original traumatic experience. Under conditions of acute fear, perception tends to narrow significantly as attention becomes focused on the immediate source of threat. As emotional arousal decreases, cognitive and perceptual fields can expand, allowing previously unnoticed elements of the situation to be recalled.
Edward was therefore asked to consider whether additional details could be remembered from the scene. Were there moments of reassurance? Was there evidence of professional competence or supportive presence, perhaps a nurse, a doctor, or a brief interaction that conveyed safety or care?
What gradually emerged was not a denial of the frightening nature of the event but a broader contextual understanding. Alongside fear and vulnerability, the memory also contained elements of medical competence, support, and human presence. These details are clinically important because they function as corrective contextual information. They allow the meaning of the memory to shift from “I was powerless and alone” toward a more integrated narrative: “I was terrified, and I was also cared for, treated, and ultimately survived”.
This process represents cognitive updating, but it is not purely intellectual. As the narrative context expands, emotional responses often shift as well. Clients frequently report subtle changes in bodily tension, breathing, or overall affect as the story becomes less narrowly defined by threat and more integrated within a broader autobiographical framework.
The “Warrior Scar” and Tattoo Message: Symbols of Safety, Identity Integration, and Meaning
Edward carried shame about his scar and what the injury appeared to imply about him. Within the Integrated-Self module, this is precisely the type of meaning targeted for therapeutic updating: not only the memory of what occurred, but the narrative the client has come to attach to it.
We therefore explored an alternative narrative: the scar as a battle scar, a “warrior scar”, not a symbol of defectiveness, but evidence of survival. This was not introduced as a slogan, but as an invitation: if the scar could speak, what might it say? Knowing that Edward was a martial arts enthusiast, we used a culturally congruent metaphor: what might a Samurai warrior say about visible scars earned in battle? Within that frame, scars are often interpreted not as signs of weakness but as symbols of endurance, resilience, and continued capacity.
Edward was asked what he had learned or gained, however unwillingly, from the experience and what message he now carried forward. His response emerged with notable clarity: I survived. I’m wiser. I’m smarter now through this experience. I feel closer to my parents. Closer to God. I appreciate life more. This moment represented more than simple reframing. It reflected integration, trauma being woven into identity without being allowed to define identity.
Such shifts rarely emerge spontaneously. More often, they are quietly prepared during earlier stages of therapy, frequently during the assessment phase, long before formal trauma processing begins.
The NA-CBT assessment stage is sometimes misunderstood as merely structured information gathering. In practice, it resembles a compassionate journey of guided discovery through the client’s life narrative. The therapist listens not only for predisposing factors, precipitating triggers, and perpetuating maintenance loops, but also, crucially, for protective factors: aspects of the individual that continue to point toward safety, connection, meaning, and agency.
This process requires genuine curiosity, not intrusive curiosity, but a steady and respectful interest in the client as a whole person rather than a bundle of symptoms. Many clinicians naturally attend to the most visible protective factors: supportive parents, partners, or close friends. These are important. Yet some of the most powerful protective factors are quieter and more symbolic, and they may easily be overlooked unless the therapist is actively attentive to them. A hobby. A sport. A personal value system. A creative outlet. A spiritual anchor. A life motto. A piece of art. A tattoo.
A subtle protective factor emerged in Edward’s assessment in precisely this way. A tattoo became visible beneath his sleeve, and when I asked about it, he described the courage he drew from a personal quote inked on his arm:
“For God has not given us a spirit of fear, but of power and of love and of self-discipline and self-control.”
Within the NNR protocol, such values are treated as identity anchors, not as beliefs imposed by therapy, but as the client’s own language of resilience and agency. The quote was revisited during processing, not as religious counselling, but as a personal resource. It helped challenge the trauma-belief cluster often associated with shame, “I am useless, weak, and vulnerable”, and supported the development of a more coherent organising belief: fear is a state, not an identity. Fear may surge, the body may react, and intrusive memories may arise; yet none of these experiences need define the self.
From a clinical perspective, what is occurring here is not simply positive thinking. Rather, it involves the deliberate recruitment of protective factors into conscious awareness, enabling them to be accessed reliably under conditions of stress. When trauma pushes individuals into survival modes, avoidance, overcompensation, or collapse, protective factors may feel distant or irrelevant. The Integrated-Self module restores access to these resources by incorporating them directly into the reconsolidation process itself. In other words, therapists do not wait until trauma processing is complete to remind the client who they are. Instead, the self is brought into the processing so that the memory is updated in the presence of agency, meaning, and safety.
This principle extends beyond Edward’s case and becomes particularly evident in grief-related trauma. In one bereavement case (details anonymised), a client discovered that his fiancée had died from an overdose and found her body in their garden, seated on a swing. The shock of that moment became a recurring flashback and “hot memory”, not only visually distressing but also morally and existentially destabilising.
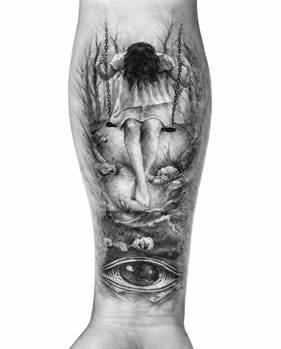
Over time, the client began to draw an image that captured his grief: a young woman seated on a swing, her posture heavy and resting, suspended within a quiet, dreamlike landscape (Figure 4 – a symbolic swing scene later modified by the addition of an eye representing continuing bond, hope, and future-oriented meaning). During assessment and subsequent therapeutic processing, the drawing was explored not only as an expression of sorrow but also as a doorway into meaning. The client later added an open eye symbol beneath the scene, his own symbolic gesture suggesting that she remained present in some form, watching over him, and that she would want him to continue living rather than disappearing into endless mourning.
The addition of the eye did not remove grief; rather, it altered the client’s relationship to grief by introducing a sense of continuing bond, care, and permission to move forward.
This example illustrates why NA-CBT places strong emphasis on protective factors, even subtle ones, during assessment and throughout Module 4. A tattoo, a drawing, a hobby, a sport, or a newly discovered passion during recovery should not be dismissed as peripheral elements. Such elements can function as NeuroAffective safety cues, anchoring attention and supporting identity integration precisely at the moment when trauma threatens to collapse the self into fear and shame.
When trauma processing achieves integration, the observable signs are often subtle rather than dramatic. Toward the end of an NNR session, a gentle clinical check question may be used: “If you look back now at the worst moment we discussed, how clear does it feel? Does it still feel as though it happened yesterday?” Clients are reassured that after successful processing, memories may feel somewhat foggier, more distant, or less emotionally vivid. This shift can initially provoke concern: “Am I forgetting?” Yet it often reflects precisely the outcome therapy aims to achieve. The memory remains accessible, but it no longer intrudes into the present with the same emotional urgency.
When Edward later reported that the hospital moment felt more distant and less vivid, accompanied by a substantial reduction in emotional intensity, the change did not represent erasure of the event. Rather, it reflected memory reconsolidation in lived form.
What Is Happening Beneath the Surface
If the NeuroAffective Narrative Reconsolidation (NNR) process is described purely in cognitive-behavioural terms, it can be understood as a structured blend of imaginal exposure, hotspot processing, somatic monitoring, cognitive updating, and meaning reconstruction. The client activates the trauma memory in a controlled therapeutic context, identifies moments of peak emotional intensity, and gradually revisits these moments while introducing new information and interpretations that modify the original meaning of the event.
If the same process is described using EMDR terminology, it resembles targeted memory activation combined with a broader or more distributed attentional stance. The client maintains contact with the trauma memory while simultaneously remaining anchored in the present through breathing, bodily awareness, imagery, and environmental orientation. This widening of attention allows the nervous system to process the memory without becoming overwhelmed. The individual is not absorbed entirely by the traumatic scene; instead, part of awareness remains grounded in present safety. This dual attentional stance, characterised by maintaining a wider field of attention rather than a narrow focus, allows the memory to be revisited while reducing the likelihood that the nervous system will interpret the experience as a current threat.
What NA-CBT adds to these traditions is an explicit emphasis on the simultaneous engagement of physiology, affect, and cognition. Trauma recovery rarely occurs through cognitive insight alone. The body is not a secondary participant in the process; it is often the first system to detect danger and the last to recognise that the danger has passed. When therapy focuses solely on thought content, the body may continue to generate threat signals that override rational understanding.
From a neurobiological perspective, trauma is encoded not only as narrative memory but also as patterns of physiological activation. Tightness in the chest, tension in the abdomen, sudden shifts in breathing or heart rate, and waves of fear or nausea can all become embedded within the memory network. When these bodily responses are triggered, they can reactivate the emotional meaning of the trauma even when the individual intellectually understands that the event is over. In such circumstances, cognitive restructuring alone may feel like attempting to reason with an alarm system that continues to sound.
For this reason, regulation within NNR is not simply preparation for processing; it is an integral component of the processing itself. When breathing slows, bodily tension decreases, and the client learns to modulate distress while recalling the memory, new physiological information becomes encoded alongside the original memory trace. The nervous system gradually learns that the event belongs to the past rather than the present.
In this sense, physiological regulation becomes the bridge that enables cognitive updating to occur.
Affect Regulation Before Processing: Why TED Matters, and How It Helped Edward
For trauma processing to be possible, clients require more than psychological insight. They require physiological capacity. This capacity partly emerges from emotional regulation skills such as grounding techniques, progressive muscle relaxation, and body scanning. However, NA-CBT also places considerable emphasis on biological regulation through lifestyle stabilisation.
In clinical practice it becomes clear that trauma frequently disrupts fundamental biological rhythms. Sleep becomes fragmented or shallow, physical activity decreases or becomes associated with threat, and dietary patterns become irregular. These disruptions amplify emotional vulnerability. A fatigued nervous system reacts more strongly to stress, struggles to regulate fear responses, and finds it more difficult to tolerate the emotional activation required for trauma processing.
This is where the TED model becomes particularly relevant. In its original formulation, TED focuses on three biological systems that often become destabilised under chronic stress: tiredness (sleep regulation), exercise, and diet (hydration). Rather than treating these as peripheral wellbeing recommendations, NA-CBT frames them as integral components of emotional regulation (Mirea, 2025a, 2025b).
In some contexts, the model is reframed and expanded, using more strength-based language such as Train – Eat – Dream. This shift is not merely cosmetic; it reflects formulation findings and a therapeutic emphasis on rebuilding physiological resilience rather than simply managing symptoms.
For Edward, the TED model became an important turning point in therapy because it helped him gradually rebuild trust in his body. Trauma had taught his nervous system that the body itself was dangerous. The injury had arrived suddenly and without warning, transforming what had once been a source of strength, his physical competence, into a site of vulnerability.
Processing trauma under such conditions can be difficult. Asking a client to revisit traumatic memories while their biological systems remain unstable is comparable to asking someone to rebuild a house while the foundations are still shifting beneath it.
We therefore began by stabilising sleep patterns. The aim was not perfection but rhythm. Edward began noticing that nights of better sleep were followed by days in which intrusive images were less vivid and his concentration improved. Even small improvements in sleep produced noticeable changes in emotional tolerance, reinforcing the importance of physiological regulation.
Exercise required particularly careful handling. For Edward, physical activity had become intertwined with threat because the injury occurred during boxing training. The gym was no longer a neutral space; it represented the moment his life changed. Rather than pushing him back toward high-intensity training, movement was reframed as a way of retraining the nervous system.
Initially this involved non-contact physical activity,exercise that communicated safety rather than competition or performance. Gentle training allowed his body to experience movement again without triggering the fear network associated with the trauma. Over time, the nervous system began to relearn a simple but powerful message: my body can move and nothing terrible happens. In this sense, exercise functioned both as behavioural activation and graded exposure within a NeuroAffective framework.
Dietary stabilisation also played an important role. Fluctuations in blood sugar, irregular eating patterns, and nutritional depletion can create physiological states that mimic anxiety or emotional instability. As Edward began eating more regularly and nourishing his body consistently, he noticed feeling less reactive and less physically unsettled. His emotional responses became more predictable and manageable.
By the time we entered Module 4 and began formal trauma processing, these physiological foundations proved essential. When Edward activated the trauma memory, he had internal resources available to regulate the experience. He could slow his breathing and genuinely experience its calming effects. He could observe bodily sensations without immediately interpreting them as signs of danger. The imagery of turning the distress dial downward became effective partly because his nervous system had already practised lowering arousal in everyday life.
From the perspective of NA-CBT, this illustrates a central principle: trauma processing is not something done to a memory in isolation. It is something done with a nervous system. The TED model helps prepare that nervous system so it can participate in the reconsolidation process rather than being overwhelmed by it.
Closing Reflections
The Development of the Integrated-Self module is often the stage in therapy where a quiet but profound shift occurs. Many clients arrive feeling fragmented, as though their lives have been divided into two incompatible chapters: the person they were before the trauma and the person they became afterwards. Even when daily functioning resumes, the memory of the event can remain emotionally unfinished, intruding into the present through flashbacks and intense physiological reactions, accompanied by an unshakeable sense that danger still exists somewhere beneath the surface.
What clients often rediscover during this phase of therapy is not perfection or invulnerability, but continuity. They become able to look back at what happened without being pulled back into it. The event becomes part of their history rather than an ongoing threat. The nervous system no longer reacts as though the trauma is unfolding in the present moment.
In simple terms, the memory becomes exactly what it is meant to be: just one of the numerous memories once again, some are good memories, some are not so great…
The NeuroAffective Narrative Reconsolidation (NNR) protocol is one way of supporting that transition. It offers a structured framework that therapists can follow and refine while remaining flexible enough to meet each client’s nervous system where it currently is. Some individuals require more time in physiological stabilisation, while others move more quickly into narrative processing. What remains constant is the principle that trauma recovery requires cooperation between body, emotion, and cognition. Reliving the story alone is not sufficient, just as sensation alone is not sufficient. Healing often occurs when both are allowed to change together.
Within this process, trauma memories are not erased or suppressed; they are integrated. Clients learn that they can revisit the past while remaining anchored in the present. The memory gradually loses its power to dictate identity or future expectations. In many cases, it even becomes a source of meaning, strength, and personal insight, an experience that has been survived, understood, and woven into a broader narrative of the self.
One observation may resonate with many clinicians. It is not uncommon to meet clients who intellectually understand that their trauma is over yet continue to react to reminders with powerful bodily responses. They may say, “I know it’s over”, while still feeling their heart race, their stomach tighten, or their breath shorten when the memory arises.
From a neurobiological perspective, the explanation is straightforward: the body learns threat before the mind has time to interpret it.
And sometimes the body must learn safety before the mind can fully believe it. Integration is often the missing link. More often than not, it begins with helping the body learn what the mind already knows: it is over.
The therapeutic shifts described in NNR are consistent with emerging research on memory reconsolidation and emotional learning. When an emotionally significant memory is reactivated under conditions of relative safety and physiological regulation, the underlying memory trace may temporarily enter a labile state in which new contextual information can be incorporated before the memory is stored again (Nader and Hardt, 2009; Lane et al., 2015). During this reconsolidation window, previously threat-coded experiences can be updated through the integration of corrective emotional information, changes in autonomic regulation, and revised cognitive meaning.
From this perspective, the combination of narrative activation, physiological regulation, and cognitive updating used in NNR may facilitate conditions under which traumatic memories become re-encoded with reduced threat intensity and improved autobiographical integration. While further empirical research is required to directly test these mechanisms within the NA-CBT framework, current findings from affective neuroscience provide a plausible explanatory model for how integrated trauma processing may occur.
Clinical Implications and Future Research
The NeuroAffective Narrative Reconsolidation protocol illustrates how trauma processing can be approached through the coordinated engagement of physiological regulation, emotional processing, and cognitive updating. For clinicians, the model highlights the importance of preparing the nervous system for trauma work through stabilisation strategies, including affect regulation skills and biological rhythm restoration such as those described in the TED framework. The integration of somatic monitoring, narrative activation, and identity reconstruction offers a structured yet flexible approach that may help clients revisit traumatic memories while maintaining sufficient regulation to allow meaningful updating to occur. Importantly, the model emphasises that trauma processing is not solely a cognitive intervention but a whole-system process involving body, affect, and meaning.
Future research is required to examine the effectiveness of NA-CBT and the NNR protocol in controlled clinical settings. Empirical studies could explore treatment outcomes across different trauma populations and compare the model with established trauma therapies such as trauma-focused CBT and EMDR. Additional research may also investigate the neurobiological mechanisms underlying change, particularly the role of physiological regulation and memory reconsolidation processes in facilitating autobiographical integration. Such investigations would help clarify the therapeutic mechanisms involved and determine the potential contribution of NA-CBT within the broader landscape of evidence-based trauma interventions.
When such integration occurs, the trauma does not disappear from the person’s history, but it loses its power to dominate the present, becoming part of a life story that can be remembered, understood, and carried forward without fear.
Key Terms
NeuroAffective-CBT (NA-CBT); NeuroAffective Narrative Reconsolidation (NNR); trauma therapy; memory reconsolidation; affect regulation; interoception; dual attention; Integrated-Self; pendulum formulation; TED (Tired-Exercise-Diet) model; TED 2.0 (Train–Eat–Dream); PTSD; autobiographical memory integration.
References
Brown, B. (2012) Daring Greatly. New York: Gotham Books.
Ehlers, A. and Clark, D.M. (2000) ‘A cognitive model of post-traumatic stress disorder’, Behaviour Research and Therapy, 38(4), pp. 319–345.
Hackmann, A., Bennett-Levy, J. and Holmes, E.A. (eds.) (2011) The Oxford guide to imagery in cognitive therapy. Oxford: Oxford University Press.
Lane, R.D., Ryan, L., Nadel, L. and Greenberg, L. (2015) ‘Memory reconsolidation, emotional arousal, and the process of change in psychotherapy: new insights from brain science’, Behavioral and Brain Sciences, 38, e1.
LeDoux, J. (2015) Anxious: Using the Brain to Understand and Treat Fear and Anxiety. New York: Viking.
Mirea, D. (2025a) The use of lifestyle interventions in psychotherapy: Why sleep, movement and metabolic stability matter. Available at: https://neuroaffectivecbt.com/2025/12/17/the-use-of-lifestyle-interventions-in-psychotherapy/ (Accessed: 18/03/2026).
Mirea, D. (2025b) TED in NeuroAffective-CBT®: An applied self-regulation framework for enhancing emotional well-being through sleep, movement and nutrition. Available at: https://neuroaffectivecbt.com/2025/12/10/ted-in-neuroaffective-cbt-an-applied-self-regulation-framework-for-enhancing-emotional-well-being-through-sleep-movement-and-nutrition/ (Accessed:18/03/2026)
Nader, K. and Hardt, O. (2009) ‘A single standard for memory: the case for reconsolidation’, Nature Reviews Neuroscience, 10(3), pp. 224–234.
Shapiro, F. (2018) Eye Movement Desensitization and Reprocessing (EMDR) Therapy. 3rd edn. New York: Guilford Press.
Clinical Note
The case illustration presented in this article is anonymised and partially modified for confidentiality. NeuroAffective Narrative Reconsolidation (NNR) is intended for use by trained mental health professionals within appropriate clinical settings.