Welcome to NeuroAffective-CBT®
NeuroAffective-CBT® is the home of evidence-based psychotherapy.. where scientific rigor meets compassion and empathy, and where real, lasting change begins.
“Psychotherapy is not simply a technique. It is an encounter between two emotional beings.
Excellent psychotherapy requires both knowledge and humanity, a therapist who is willing not only to understand your experience, but to feel its weight alongside you.” – Daniel Mirea
Understanding the Landscape
To see where NeuroAffective-CBT fits, it helps to step back and take a bird’s-eye view of the psychotherapy landscape. Imagine three overlapping circles, each representing one of the field’s major traditions..
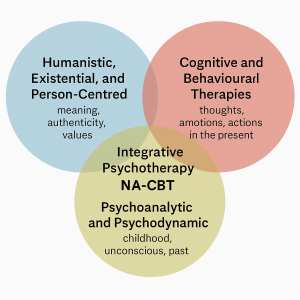
Humanistic, existential, and person-centred therapies,
focusing on meaning, authenticity, values, and the lived experience of being human.Psychoanalytic and psychodynamic therapies,
exploring childhood, attachment, unconscious processes, and the enduring influence of the past.Cognitive and behavioural therapies (CBT and its many branches),
targeting thoughts, emotions, and actions in the present.
Where these circles intersect lies the heart of modern psychotherapy. After all, one cannot meaningfully change thoughts or behaviours without understanding a person’s history, values, and aspirations. Likewise, exploring meaning and existence without acknowledging early emotional experiences leaves an incomplete picture. Even psychoanalysis, with its deep focus on the past, ultimately seeks to shape behaviour and choice in the present and future.
The Beauty of Integration
If this sounds intricate, it’s because the field of psychotherapy is wonderfully complex. Different schools of therapy take different paths. Some require years of exploration; others work within weeks or months. Yet all share the same fundamental goal: to help people suffer less, understand themselves more deeply, and live more fully.

NeuroAffective-CBT (NA-CBT) belongs to the broad family of cognitive-behavioural therapies, known for their structured frameworks, clear boundaries, and strong empirical foundations. What distinguishes NA-CBT is its depth of integration. It weaves together neuroscientific understanding, affective and relational insight from psychodynamic and humanistic traditions, and the practical, outcome-focused methods of behavioural science.
Here, philosophy meets science. The body meets the mind.
Mind, Body, and the Foundations of Change
Many clients enter psychotherapy believing their distress is “all in the mind”. From a NeuroAffective-CBT perspective, this view is incomplete.
Mind and body form a single regulatory system. Emotional suffering often emerges from the interaction between physiological states and learned affective patterns.
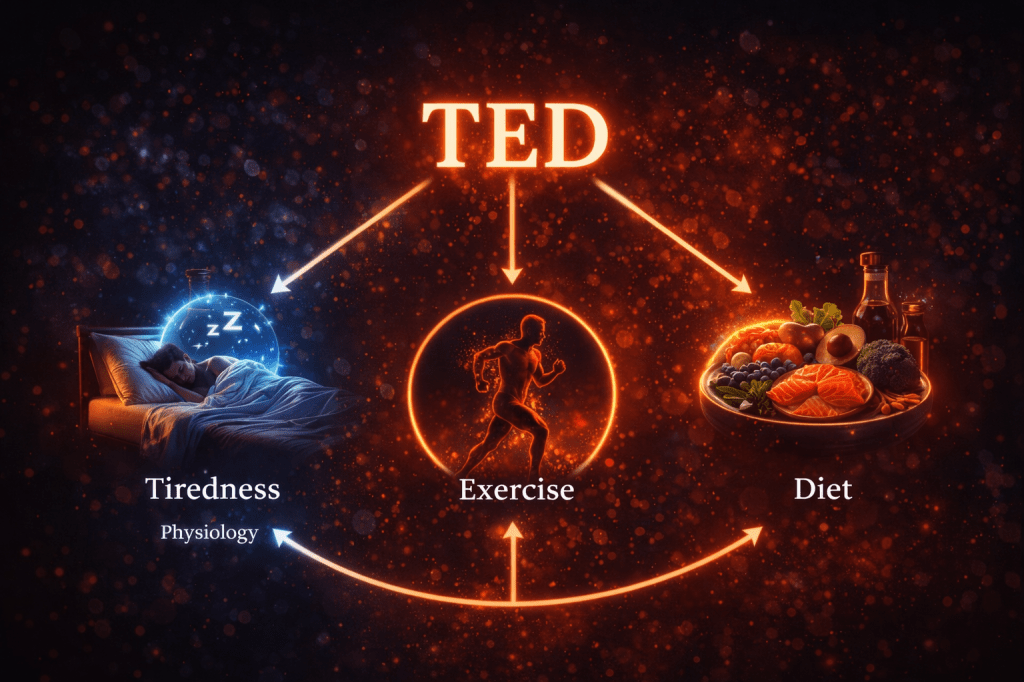
For this reason, NA-CBT integrates TED — Tiredness, Exercise, and Diet — as a core stabilisation framework within psychotherapy.
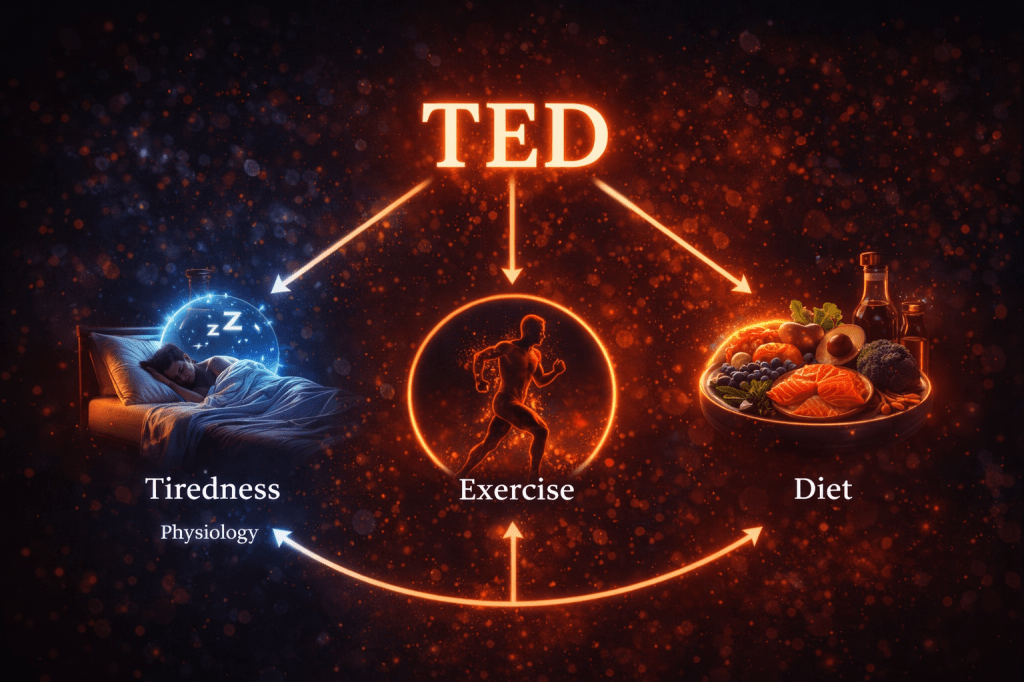
TED addresses the physiological ground on which thoughts, emotions, and relationships unfold.
NA-CBT is grounded in a central principle: the brain’s core function is prediction in the service of protection. The nervous system is constantly asking: “Am I safe? What is about to happen? How bad could it be?” These predictions are shaped not only by conscious beliefs and interpretations, but by bodily signals, sleep, movement, metabolic stability, and neurochemical balance.
When physiology is unstable, predictive systems become threat-sensitive. Neutral events are more easily experienced as dangerous. Shame activates more quickly. Emotions intensify and linger.
TED is not a wellness add-on. It is often the stabilising platform that makes deeper cognitive, emotional, and relational work possible.
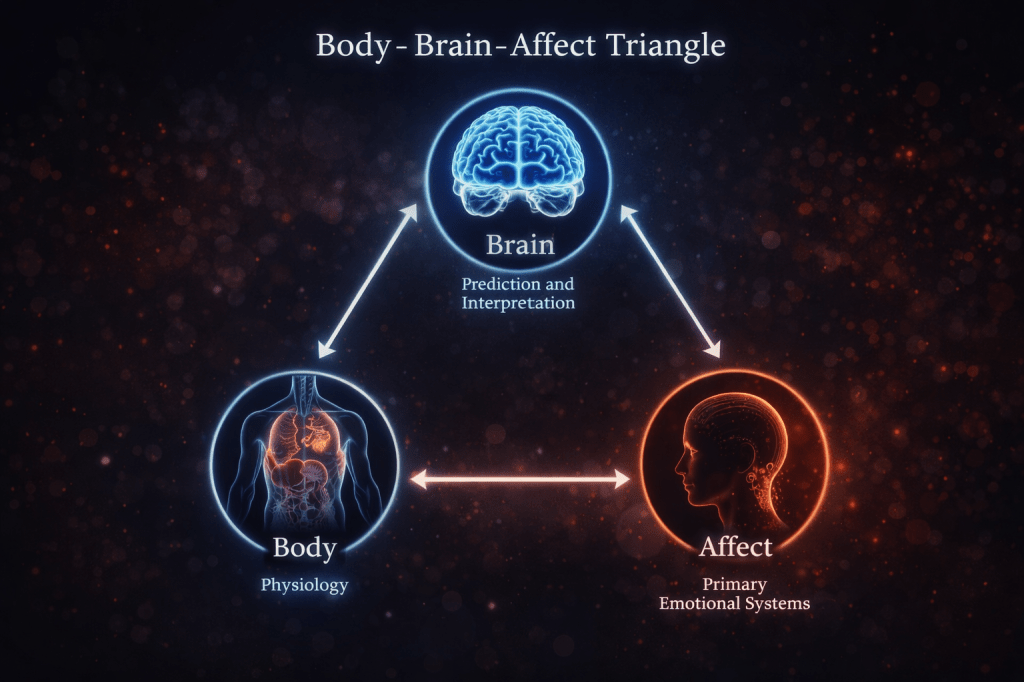
The Body–Brain–Affect Triangle
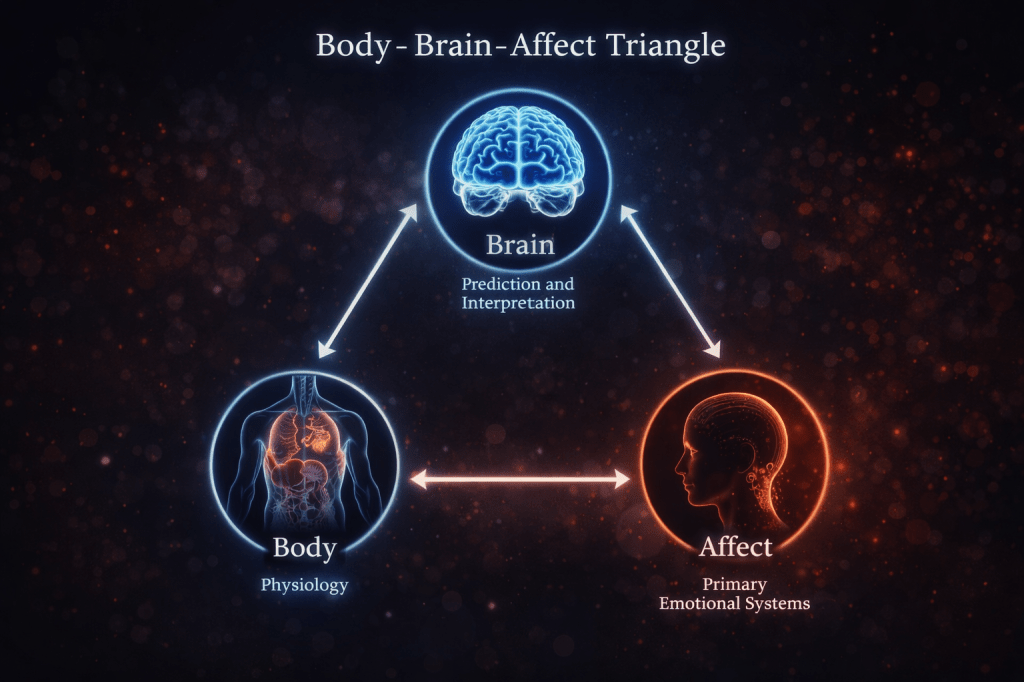
Central to NeuroAffective-CBT is the Body–Brain–Affect triangle — a dynamic system in which each component continuously influences the others.
Body (Physiology)
Sleep, energy, movement, nutrition, hormonal balance, and nervous system activation provide the biological context in which experience unfolds.
Brain (Prediction and Interpretation)
The brain continuously anticipates potential threats and prepares the organism to respond, constructing meaning from bodily signals and emotional states.
Affect (Primary Emotional Systems)
Fast, survival-oriented responses such as fear, shame, anger, and relief shape attention, behaviour, and self-experience.
Influence flows in all directions. A shift in any one corner alters the entire system.
Within this triangle, TED functions as the physiological regulation arm of NA-CBT, reducing background volatility so deeper psychological learning can occur.
Differentiating Affect from Interpretation
A central therapeutic aim of NeuroAffective-CBT is helping clients distinguish between:
- Raw affect — the body’s immediate signal of threat, pain, or unmet need
- Interpretation — the meaning the mind assigns to that signal
When affect and interpretation collapse into one another, emotions feel overwhelming, self-defining, or dangerous. People begin to experience what they feel as what they are.
TED slows this process by first asking a more fundamental question:
What is the body signalling right now? Is the reaction accurately calibrated to the present situation?
By stabilising physiological regulation, NA-CBT creates the conditions in which emotions can be felt without being feared, and meanings can be explored without being dictated by threat.
NeuroAffective-CBT and the Emerging “Fourth Wave”
Within the broader cognitive-behavioural tradition, NeuroAffective-CBT can be understood as part of an emerging process-based “fourth wave” of psychotherapy, integrating neuroscience, physiology, lifestyle science, and embodied experience into psychological treatment.
At its core lies a simple biological reality: the brain evolved in the service of survival. Its primary task is not abstract reasoning, but anticipation, detecting potential danger and preparing the organism before threat fully unfolds.
While earlier waves of CBT emphasised behaviour, cognition, and acceptance, NA-CBT places affective underlayers — such as shame, internal threat, and self-loathing — at the centre of formulation and intervention. Affect is fast, precognitive, and survival-driven. Cognition is the meaning-making layer built upon it.
Because the brain is fundamentally organised around prediction and protection, emotional responses often emerge before conscious thought. By working at this deeper regulatory level, NeuroAffective-CBT bridges science and meaning, body and mind, insight and lived experience, offering a psychotherapy that is both deeply human and rigorously evidence-based.